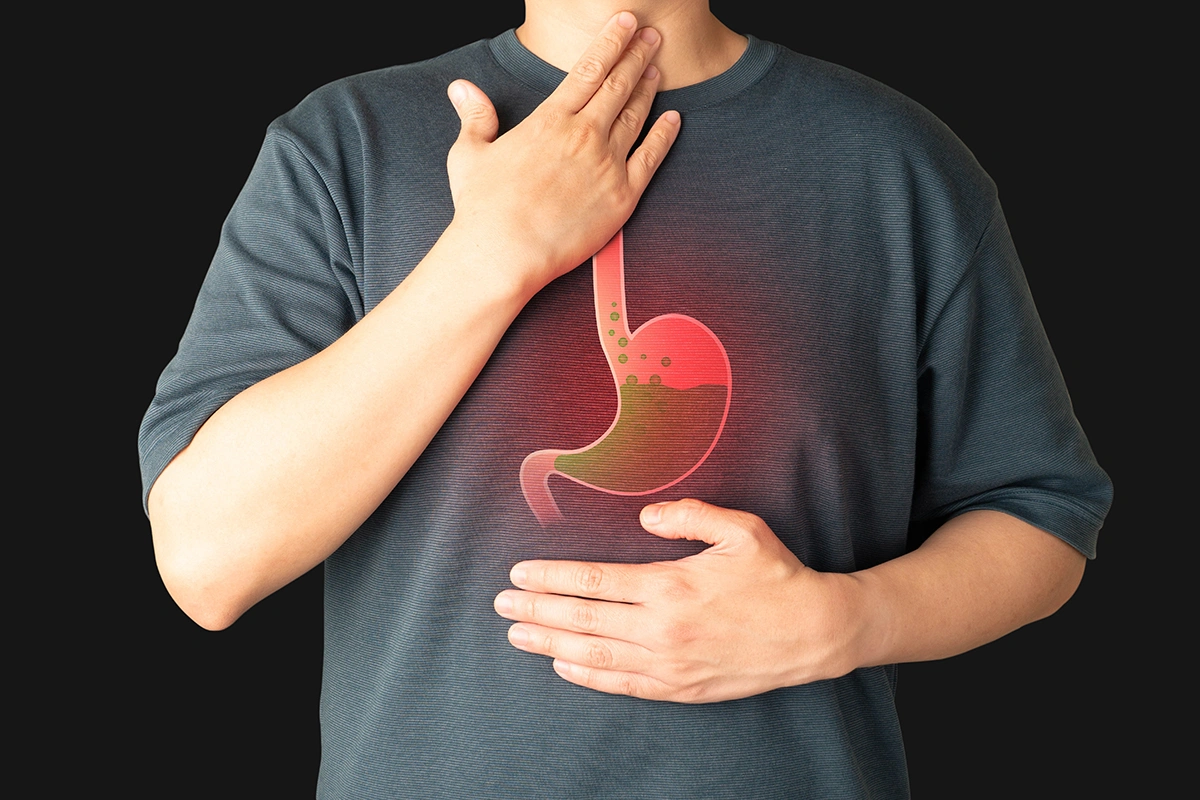

Gastroesophageal reflux disease (GERD) is a chronic form of acid reflux where stomach acid frequently flows back into the oesophagus. Symptoms that occur more than twice a week, persist despite lifestyle changes, or affect swallowing or the throat may indicate GERD and require medical evaluation.
What Is the Difference Between Acid Reflux and GERD?
Acid reflux refers to the occasional backflow of stomach acid into the oesophagus. It is common and often triggered by large meals, certain foods, or lying down after eating.
GERD is a chronic condition where acid reflux occurs frequently (typically more than twice a week) or causes persistent symptoms.
Although the terms are often used interchangeably, acid reflux and GERD are not the same. Acid reflux is occasional and usually harmless, while GERD may require ongoing management.
Feature | Acid Reflux | GERD |
Frequency | Occasional | Frequent (more than twice a week) |
Severity | Usually mild and temporary | Persistent or worsening symptoms |
Cause | Often triggered by diet or lifestyle | Often due to a weakened lower oesophageal sphincter (LES) |
Symptoms | Heartburn, occasional discomfort | Heartburn, regurgitation, swallowing issues, throat symptoms |
Duration | Short-term | Long-term (chronic condition) |
Treatment | Lifestyle changes | May require medication or procedures |
Signs Your Acid Reflux May Have Progressed to GERD
Not all reflux is a cause for concern. However, the following signs suggest it may have developed into GERD:
- Frequent heartburn (more than twice a week)
- Acid regurgitation (sour or bitter taste in the mouth)
- Chest discomfort or burning sensation
- Difficulty swallowing or a feeling of food being stuck
- Chronic cough or throat irritation
- Hoarseness or voice changes
- Symptoms that worsen at night or when lying down
Symptoms may vary between individuals. Some people experience mainly chest symptoms, while others notice throat or respiratory issues.
Why Does GERD Develop?
GERD occurs when the normal barrier between the stomach and oesophagus is disrupted.
Common contributing factors include:
- Weak or relaxed LES: Allows acid to flow upward
- Increased abdominal pressure: Often due to obesity or pregnancy
- Hiatal hernia: Part of the stomach moves above the diaphragm
- Delayed stomach emptying: Keeps acid in the stomach longer
Several everyday habits and foods can trigger or worsen GERD symptoms, including:
- Fatty or spicy foods
- Caffeine (coffee, tea)
- Alcohol
- Smoking
- Eating large meals or lying down soon after eating
What Happens If GERD Is Left Untreated?
Untreated GERD can lead to complications over time due to ongoing irritation of the oesophagus.
Possible complications include:
Oesophagitis
Inflammation of the oesophageal lining caused by repeated exposure to stomach acid. This can lead to symptoms such as pain when swallowing, chest discomfort, or worsening heartburn. Over time, untreated inflammation may damage the lining and increase the risk of further complications.
Strictures
Narrowing of the oesophagus due to repeated acid-related injury and healing. Scar tissue forms, which can make swallowing difficult and cause food to feel stuck in the throat. In more severe cases, medical procedures may be needed to widen the oesophagus.
Barrett’s Oesophagus
A condition where the normal lining of the oesophagus changes in response to long-term acid exposure. This change itself does not cause symptoms but is significant because it is associated with an increased risk of oesophageal cancer. Regular monitoring may be recommended for affected individuals.
Early recognition and management can reduce the risk of these complications.
How Is GERD Diagnosed?
GERD is often diagnosed based on symptoms and medical history. However, if symptoms are persistent, unclear, or do not respond to treatment, further evaluation may be needed to confirm the diagnosis and assess for complications.
Common diagnostic methods include:
Upper Endoscopy
A thin, flexible camera is used to examine the lining of the oesophagus and stomach. This test can identify inflammation, ulcers, or changes such as Barrett’s oesophagus, and helps assess the severity of damage caused by acid reflux.
pH Monitoring
This test measures how often and how long stomach acid enters the oesophagus over a 24-hour period. It is particularly useful when symptoms are not typical or when the diagnosis is uncertain.
Oesophageal Manometry
This test evaluates how well the muscles of the oesophagus and the lower oesophageal sphincter (LES) are functioning. It helps determine whether abnormal muscle movement is contributing to reflux symptoms.
These tests help confirm the diagnosis and guide treatment decisions.
How Is GERD Treated and Managed Effectively?
GERD is typically managed in a stepwise approach, starting with lifestyle changes and progressing to medication or procedures if symptoms persist.. The goal is to reduce acid reflux, relieve symptoms and prevent complications.
Lifestyle changes
For many people, simple daily habits can make a big difference:
- Adjust your diet: Avoid trigger foods like spicy, fatty, or acidic meals.
- Eat smaller meals: Large portions can increase pressure on the stomach.
- Don’t lie down after eating: Wait at least 2–3 hours before sleeping.
- Maintain a healthy weight: Reduces pressure on the stomach.
- Elevate your head while sleeping: Helps prevent acid from flowing back up.
Medications
If lifestyle changes aren’t enough, medications may be recommended:
- Antacids: Provide quick, short-term relief.
- H2 blockers: Reduce acid production.
- Proton pump inhibitors (PPIs): More effective for long-term acid control.
Minimally invasive procedures and surgery
For patients with persistent symptoms or complications, further treatment may be needed:
- LINX procedure: A small ring of magnetic beads is placed around the lower esophagus to strengthen the valve and prevent acid reflux.
- Fundoplication surgery: The upper part of the stomach is wrapped around the esophagus to improve the function of the valve.
How Do You Know Which Treatment You Need?
GERD treatment is usually guided by symptom severity and response to initial measures:
- Mild symptoms: Often managed with lifestyle changes alone
- Persistent symptoms: May require medication such as PPIs
- Severe or long-standing GERD: Further evaluation and procedures may be considered
A specialist assessment helps determine the most appropriate treatment based on the underlying cause and severity.
Achieve Long-Term Relief from GERD with Dr Shanker
GERD is a common but manageable condition when recognised early and treated appropriately. By understanding its symptoms, causes, and treatment options, you can take simple steps to reduce discomfort and improve your daily life. If symptoms persist, seeking medical advice can help prevent complications and ensure proper care.
Here at Digestive Centre, patient care and treatments are aimed at improving health and quality of life with lasting results. Under the leadership of Dr Shanker Pasupathy who has undergone advanced training in laparoscopic and robotic surgery in Europe, patients benefit from advanced diagnostics and treatment options including the LINX procedure and fundoplication surgery. If you are experiencing ongoing reflux symptoms, a specialist evaluation can help determine a personalised treatment approach for effective, long-term relief.
FAQs About When Acid Reflux Becomes GERD
Your Dedicated Specialist
Dr Shanker Pasupathy
Upper Gastrointestinal & Bariatric Surgeon
MBBS, National University of Singapore
Fellow of the Royal College of Surgeons (Glasgow)
Fellow of the Royal College of Surgeons (Edinburgh)
Dr Shanker Pasupathy is the Medical Director of the Digestive Centre at Mount Elizabeth Hospital and a recognised key opinion leader in gastro-oesophageal reflux, hernia and metabolic disease management. He has extensive international training in gastrointestinal endoscopy, laparoscopy and robotic surgery, with experience gained in the UK, France and Germany.
Prior to private practice, he was Director of the LIFE Centre and Senior Consultant at Singapore General Hospital, where he led the metabolic-bariatric surgery service. Dr Shanker is actively involved in training healthcare professionals across the region and was awarded the Dean’s Award for teaching excellence from NUS Medicine. He also holds leadership positions in regional surgical societies and is a member of the American Society for Metabolic and Bariatric Surgery (ASMBS).
We offer comprehensive, personalised care for acid reflux and obesity.
Please fill in the form to enquire or book an appointment here. We’ll get back to you as soon as possible.
Mount Elizabeth Hospital3 Mount Elizabeth #12-14 Mount ElizabethMedical Centre Singapore 228510
Tel: +65 6737 5388Whatsapp: +65 8799 2791
Opening Hours:
Mon-Fri: 9am - 5pmSat: 9am - 12.30pmClosed on Sunday & Public Holidays


